Breastfeeding offers countless benefits for both mother and baby, but it’s not without its challenges. One of the more painful and frustrating conditions breastfeeding mothers may encounter is mastitis. Understanding what mastitis is, how to recognize the symptoms, and what steps to take for relief and prevention can make a significant difference in the breastfeeding journey.
What is Mastitis?
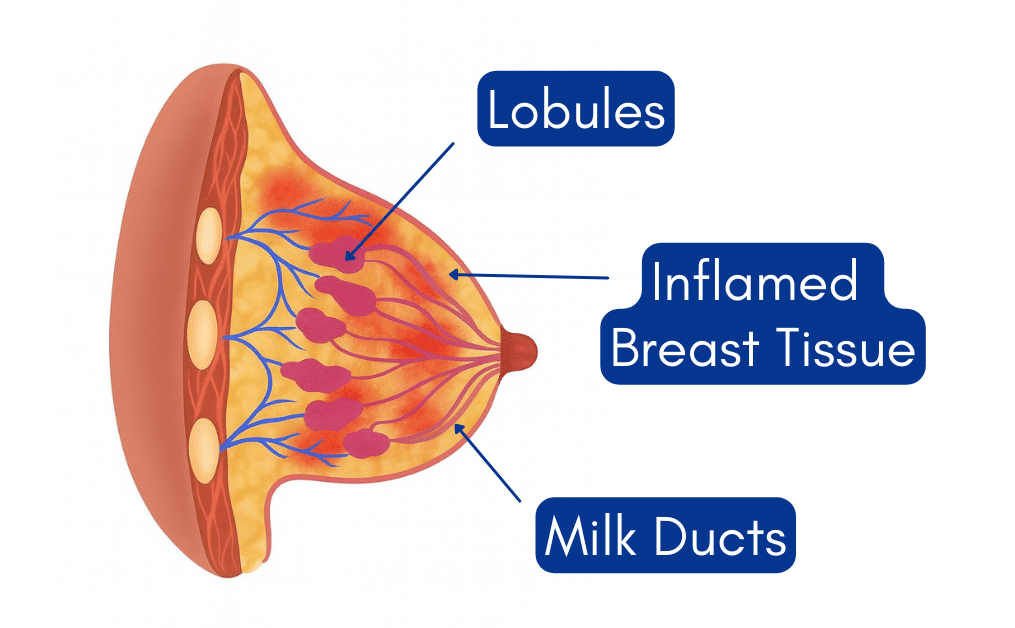
Mastitis is an inflammation of the breast tissue, often caused by a blocked milk duct or bacterial infection. It typically affects one breast and can appear suddenly, bringing with it pain, swelling, warmth, and sometimes fever or flu-like symptoms. Mastitis most commonly occurs within the first few weeks after birth but can develop at any point during lactation.
There are two main types of mastitis:
Non-infectious mastitis: Usually caused by milk stasis (when milk isn’t properly drained from the breast).
Infectious mastitis: Occurs when bacteria enter the breast tissue, often through a cracked nipple, leading to infection.
How Common is Mastitis?
Mastitis is relatively common among breastfeeding mothers:
10%–20% of breastfeeding women will experience at least one episode.
It is most likely to occur within the first 6 to 12 weeks postpartum, though it can happen at any stage of lactation.
First-time moms and those with latching or milk drainage issues are more at risk.
While mastitis can be discouraging, knowing how to identify and treat it early can help mothers continue breastfeeding successfully.
Signs and Symptoms
Early detection of mastitis can help prevent complications and support continued breastfeeding. Common symptoms include:
A hard, sore lump in one area of the breast
Redness, warmth, and swelling on the affected breast
Pain or burning during breastfeeding or in between feedings
Flu-like symptoms such as fever, chills, fatigue, or body aches
Decreased milk supply in the affected breast
Tender or cracked nipples
It’s important to note that mastitis is different from engorgement or plugged ducts, although they can feel similar and may lead to mastitis if not resolved.
What Causes Mastitis?
Mastitis often results from a combination of factors:
Ineffective milk removal: Infrequent feedings, latching issues, or abrupt weaning can cause milk to accumulate.
Blocked ducts: When milk flow is restricted, pressure builds up, causing inflammation.
Nipple damage: Cracks or irritation can create an entry point for bacteria, leading to infection.
Stress and fatigue: Both physical and emotional stress can suppress immune function and contribute to inflammation.
Treatment and Relief
The good news is that mastitis can usually be managed effectively at home, especially when caught early. Here are steps breastfeeding moms can take:
1. Continue Breastfeeding or Pumping
It may be painful, but regular milk removal is crucial. Try to nurse on the affected side first and ensure a deep latch. If nursing is too painful, gently express or pump the milk.
2. Apply Heat and Massage
Warm compresses or a warm shower before feeding can help open ducts and improve milk flow. Use gentle massage starting from behind the lump and moving toward the nipple.
3. Rest and Hydration
Prioritize rest as much as possible and drink plenty of fluids. Your body needs energy and hydration to fight inflammation and recover.
4. Pain Management
Over-the-counter medications like ibuprofen or acetaminophen can reduce pain and inflammation. Always consult with your care provider before taking any medication while breastfeeding.
5. Antibiotics (If Needed)
If symptoms persist beyond 24–48 hours, or you develop a fever, your healthcare provider may prescribe antibiotics. It’s important to complete the full course, even if you start feeling better before it’s finished.
When to Seek Medical Help
Contact your healthcare provider if you:
Have a fever over 101°F (38.5°C)
See pus or blood in your milk
Experience symptoms that worsen or don’t improve within 48 hours
Develop mastitis repeatedly
Preventing Mastitis
While mastitis can’t always be avoided, these strategies may reduce the risk:
Ensure proper latch and positioning
Avoid long gaps between feedings
Switch nursing positions to help drain different areas of the breast
Use gentle breast massage if you feel a lump or fullness
Treat nipple soreness or cracks early
Wear well-fitting, non-restrictive bras
Don’t skip pumping or nursing sessions
Emotional Support and Encouragement
Experiencing mastitis can feel discouraging, especially for new moms already adjusting to the demands of breastfeeding. It’s important to know that mastitis is common and does not mean breastfeeding must end. With the right care and support, most mothers recover quickly and continue to breastfeed successfully.
If you need guidance or emotional reassurance, consider connecting with a lactation consultant, Hypnobabies birth professional, or a local breastfeeding support group. You’re not alone, and help is available.
Resources:
Mastitis is tough, but so are you. With knowledge, support, and self-care, you can continue your breastfeeding journey with confidence. 🧡
Search
Categories
- Birth Center Stories 111
- Birth Hypnosis 33
- Birth Professionals 34
- Breech Babies 23
- Childbirth Education 55
- First Time Moms 198
- Home Birth 184
- Hospital Birth 500
- Hypnobabies Blog 198
- Inductions 70
- Know Your Options 95
- Media Library 21
- Multiples 18
- News 60
- Podcasts 2
- Pregnancy Hypnosis 25
- Start Here 24
- Uncategorised 34
- VBAC Birth 80
- Videos 31
- Water Birth 176


